What Is Twin Reversed Arterial Perfusion (TRAP) Sequence?
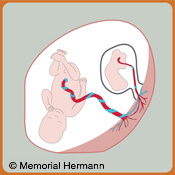
As a result, the acardiac/acephalic twin receives all of its blood from the normal or "pump" twin. In a normal fetus, arterial blood is pumped from the fetus to the placenta for oxygenation from the mother (placental bed). Because the abnormal fetus does not have a heart, all of its blood must come from the normal twin.
This abnormal twin is kept alive by blood that is pumped from the normal twin through the placenta utilizing arteries to pump blood in a 'reversed' direction to the abnormal twin (TRAP sequence). As a result, the heart of the pump twin does extra work to sustain both fetuses and is at risk for heart failure.
TRAP sequence occurs in approximately 1% of monochorionic twin pregnancies and 1 in every 35,000 live births.
What Will Happen During Pregnancy?
Once the condition has been detected, a targeted ultrasound will be performed to rule out the presence of anomalies in the normal or "pump" twin. Amniocentesis will be recommended to look for chromosomal abnormalities and a specialized ultrasound of the fetal heart, called an echocardiogram, may also be performed. If left untreated, the normal twin will continue to pump blood to sustain the acardiac/acephalic twin. If the abnormal twin is large, the normal twin may develop heart failure from the additional work required to sustain itself and the acardiac/acephalic twin. The risk of heart failure and death depends on the size and burden of the abnormal fetus on the heart of the normal twin. The larger the abnormal twin, the harder the normal twin's heart must pump. If heart failure is untreated, the normal twin will not survive in 50-75% of cases.
Twin pregnancies with TRAP sequence are also at risk for premature delivery. Because the normal twin continues to pump blood to the acardiac/acephalic twin, there is increased blood flow to the kidneys resulting in extra production of fetal urine (amniotic fluid). This excess of amniotic fluid (hydramnios) can lead to preterm labor.
Your pregnancy will be closely monitored by ultrasound examinations. Some pregnancies may continue without any problems if the abnormal twin is small and does not put a lot of stress on the normal twin. Ultrasound will be used to detect signs of heart failure and stress on the normal twin. If signs of heart failure are detected and the pregnancy is far enough along, your doctors at the Center may recommend delivery. If this problem is diagnosed early in pregnancy, fetal intervention is usually may be considered to save the normal twin.
Will a Fetal Treatment Be Required?
Not every pregnancy with this condition will require fetal treatment. If it is determined that fetal intervention is the best option for your pregnancy, the team at the Center will develop a comprehensive plan for you and your baby during and after pregnancy.
The goal of fetal intervention for a twin pregnancy with TRAP sequence is to stop the abnormal blood flow from the normal twin to the abnormal twin without injuring or harming the viable (normal) fetus. Several techniques have been utilized to accomplish this goal including removing the abnormal twin, clotting the blood vessels between the twins, and ligating or cutting the cord of the abnormal twin.
Other Treatment Options
Radio-Frequency Ablation (RFA) is often used to stop the blood flow to the abnormal twin. RFA uses a thin needle-like device that is placed through the maternal abdomen and uterus into the abnormal fetal umbilical cord in order to stop the blood flow under ultrasound guidance.
The procedure is typically performed under spinal anesthesia. Afterwards, the mother is admitted to the Women's Center at Children's Memorial Hermann Hospital to monitor the pregnancy for complications. After discharge, mothers are followed by the Center as well as their obstetrician for ongoing care.
Utilizing RFA to treat TRAP sequence has been shown to be extremely effective. Our colleagues at the University of California, San Francisco have reported a success rate of greater than 90% survival of the normal twin with an average gestational age at delivery of 35 weeks.
What Special Considerations Should Be Made for Delivery?
Type of delivery: Typically, TRAP sequence does not require cesarean delivery unless an obstetric indication arises. The need for fetal intervention should not impact your mode of delivery. The delivery plan will be carefully discussed with you and your obstetrician.
Place of delivery: If all of the prenatal monitoring suggests that your baby is doing well, the baby can be delivered at the hospital of your choice. However, the hospital should be prepared to handle any intensive care needs of your newborn and have a neonatal intensive care unit with the capability to provide specialized care.
Time of delivery: Unless there are signs of fetal heart failure due to the TRAP sequence, there is no reason to intentionally induce early delivery. Early delivery may be recommended by your team at the Center for pregnancies that appear to be in danger.
What Will Happen at Birth?
Immediately following delivery, doctors will carefully evaluate your neonate. Most infants will be born without any problems. You and your loved ones should be able to immediate hold and bond with your newborn. For infants that appear to be having problems at birth, the baby will be stabilized in an intensive care unit and will be treated by the neonatologists, specialists in critically ill newborns.
Contact Us
When you contact The Fetal Center, you will be in touch with a dedicated coordinator who will walk you through the process step-by-step and help you to understand every aspect of your care.
The Fetal Center at Children's Memorial Hermann Hospital
UT Professional Building
6410 Fannin, Suite 210
Houston, Texas 77030
Phone: (832) 325-7288
Toll free: (888) 818-4818
Fax: (713) 383-1464
Email: thefetalcenter@memorialhermann.org
To contact The Fetal Center at Children's Memorial Hermann Hospital, please fill out the form below.