Pediatric orthopedic specialists make treatment decisions based on the potential for progression, which depends on three things: skeletal maturity (age), curve magnitude and location of the curve. Children who are being followed by a doctor for progression are usually seen every four to six months.
| Degree |
Treatment |
|
Less than 25 degrees
|
Periodic exams to detect progression
|
|
25 to 45 degrees in the thoracic spine
|
Brace wear
|
|
25 to 40 degrees in the lumbar spine
|
Brace wear
|
|
Greater than 50 degrees
|
Surgical correction
|
According to the Scoliosis Research Society, neither exercise nor chiropractic manipulation have been clinically documented in the management of scoliosis.
Bracing for Scoliosis
Pediatric orthopedists affiliated with Children’s Memorial Hermann Hospital strive first for nonsurgical treatment of AIS, which is why early detection is so important. While most cases have little or no medical or cosmetic significance, about 2% to 3% progress enough to require brace wear to stop the progression or surgery to correct it.
Bracing is recommended for thoracic curves 25-45 degrees during growing years. The goal of bracing is to prevent progression, rather than to correct the curve.
Most children and adolescents who qualify for bracing are fitted with a thoraco-lumbar-sacral orthosis (TLSO), constructed of advanced plastics and custom molded to exactly match the curve pattern of the spine. While there are many types of braces, the most common is the Boston brace, which extends from below the breast to the beginning of the pelvic area in front and just below the shoulder blades to the middle of the buttocks in the back.
The brace is designed to keep the lumbar area of the body in a flexed position by pushing the abdomen in and flattening the posterior lumbar contour. Pads are strategically placed to provide pressure to the curve to prevent its progression. The Boston brace can be worn under clothing without being noticeable and can be removed easily to allow children to participate in sports.
Doctors recommend brace wear for 20 to 23 hours a day, with some modification made for athletic activity. It’s important for children with scoliosis to continue to be children, and participating in sports and dance helps in their physical, social and emotional development.
In 1985, the Scoliosis Research Society conducted a clinical trial at treatment centers around the world. The study compared treated and untreated patients of the same age, curve pattern and curve severity. It produced statistical results that showed that fulltime bracing stops the progression of 80% of spinal curves.
How Long Do Children Wear the Brace?
Children wear the brace until they have stopped growing. In girls, growth usually stops between 18 months and two years after the onset of menstruation. In both boys and girls, cessation of growth is determined by a bone-age x-ray of the left wrist.
When Is Surgery Recommended?
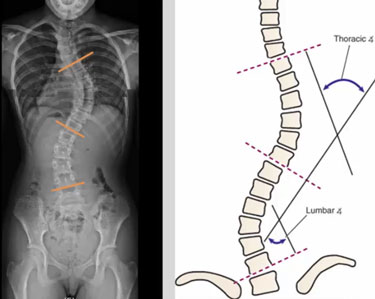
When curve magnitude reaches 45 to 50 degrees or greater in previously untreated children or in those who show no improvement with bracing, surgery is recommended. The primary goal of surgery is correction of the curve and prevention of curve progression. Larger curves are more likely to progress into adulthood and cause future back problems and other health issues.
Today, the majority of AIS cases are treated with a fusion of the affected areas and instrumentation that straightens the spine and supports the area of fusion. Posterior instrumentation may include multiple screws that attach to the pedicles of the vertebrae and multi-level hooks, which are connected to two rods and rotated to allow for correction of the curve. This approach preserves lumbar segments, resulting in greater mobility of the lumbar spine.
What Can We Expect After Surgery?
Most AIS patients do not require postoperative casting or bracing, and are usually discharged five to seven days after surgery. A research study published in the European Spine Journal in 2013 suggests that posterior correction of thoracic AIS with pedicle screw instrumentation is safe and produces a long-term stable correction and high patient satisfaction.
A study published in Scoliosis in 2015 evaluated the long-term health-related outcomes in AIS patients treated with the Boston brace or posterior spinal fusion during adolescence for curves less than 40 degrees. No clinical progression of the curve was detected during the 25-year follow-up period.