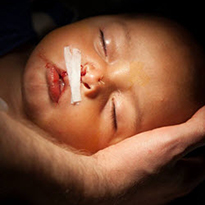
Neal Wille’s Path to a Big Smile
May 12, 2022
Three-year-old Neal Wille is among the one in 700 kids annually around the world born with a cleft lip and palate. Today, he’s a ball of smiles and sunshine when his parents bring him to see the Texas Cleft-Craniofacial Team for follow-up care after his surgeries that were performed at Chil...