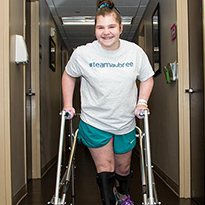
Ripp’s story: Family credits Children’s Memorial Hermann Hospital’s affiliated trauma team and TIRR Memorial Hermann for son’s recovery from a traumatic brain injury following a tractor accident.
May 19, 2023
On September 24, 2022, Chase and Kendall had a few friends over at their family farm in El Campo where they gathered around the fire pit, grilling fajitas. It was supposed to be a fun and relaxing afternoon on the farm. But then, in a matter of minutes, everything changed so quickly. Ripp had bee...